What are Functional Disorders of the Pelvic Floor?
Functional disorders of the pelvic floor include pelvic organ prolapse, chronic constipation and incontinence. They are common health problems, particularly in women. It is estimated that more than 15% of women who have had 2 or more children are affected by some form of pelvic floor disorder, which significantly affects their quality of life. Patients are often reluctant to seek medical help due to embarrassment or a mistaken perception that nothing can be done.
Why is Dynamic MRI of the Pelvic Floor a useful examination?
Dynamic MRI of the Pelvic Floor, also known as MR Defecating Proctography, is an excellent tool for assessing the entire pelvis and is particularly valuable in identifying which patients might benefit from surgical as opposed to conservative treatment. It can also assist in planning the most appropriate surgical approach. Evaluating the pelvic floor with MRI has the added benefit that patients do not receive radiation.
What disorders can Dynamic MRI of the Pelvic Floor identify?
Dynamic pelvic floor MRI can assist in the diagnosis of the following conditions:
Cystocele
Urethral hypermobility
Uterine or vaginal vault prolapse
Descending perineal syndrome
Enterocele
Peritoneocele
Rectocele
Rectal invagination and prolapse
Spastic pelvic floor syndrome or anismus
What happens when a patient has a Dynamic MRI of the Pelvic Floor?
Prior to the MRI examination, a radiographer or radiologist will explain the procedure to the patient, answering any questions or concerns they may have. The patient then changes into a hospital gown. In a private room within the radiology department, a phosphate enema will be injected into the patient’s rectum, to help cleanse the rectum prior to the examination. This involves a cupful of clear liquid being injected into the rectum whilst the patient lies on their side. A toilet is located nearby for the patient’s sole use. Once the rectum is empty, the patient enters the MRI scanner, lying down on the scanner bed on top of absorbent paper sheets. The radiologist then fills the patient’s rectum with a clear clean lubricant jelly. Imaging commences with the patient lying still within the MR scanner. After approximately 5 minutes the patient is then asked to empty their bowel on to the absorbent paper whilst we continue to scan their pelvis. Following the examination, the patient will be able to use the toilet again, before getting dressed. There are no restrictions to a patient’s daily activities following this investigation and they may return to their place of work, if they so wish.
Whilst this procedure sounds rather dirty and unpleasant, this is not the case, because the rectum will have been cleansed prior to the procedure with the insertion of the enema and the patient will be passing clean lubricant jelly during the scan.
Dynamic MRI of the Pelvic Floor is supervised and reported by Dr. Kelly MacDonald
Dynamic MRI of the Pelvic Floor is currently available for NHS patients at the Royal United Hospital, Bath and for private patients at BMI Bath Clinic, Combe Down, Bath.

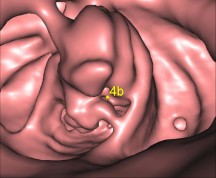 In the UK, colorectal cancer is the second most common cancer in women and the third most common in men. CT Colonography is a very well-established technique that uses a fast CT scanner to produce 2- and 3-dimensional images of the entire colon and rectum. It is fully recognized by NICE as a useful test to detect abnormalities of the large bowel, such as polyps and colorectal cancer, in symptomatic and at-risk screening patients.
In the UK, colorectal cancer is the second most common cancer in women and the third most common in men. CT Colonography is a very well-established technique that uses a fast CT scanner to produce 2- and 3-dimensional images of the entire colon and rectum. It is fully recognized by NICE as a useful test to detect abnormalities of the large bowel, such as polyps and colorectal cancer, in symptomatic and at-risk screening patients.